Manage Your Pain: Practical and Positive Ways of Adapting to Chronic Pain - Michael K. Nicholas, Allan Molloy, Lee Beeston, Lois Tonkin (2012)
Chapter 11. Challenging Ways of Thinking About Pain
Persisting pain affects different people differently. For some, persisting pain can be extremely debilitating. For others, it is something they manage without much interference in their daily lives. While just about everyone with persisting pain gets distressed about it at times, they are not always distressed about it. So we have to ask, why do some find persisting pain disabling while others don’t, and why do most people with such pain find it distressing at times but not other times.
One reason is that their pain is not always so bad. Generally, when pain is only mild it is not as troubling as when it is very severe. But research on chronic pain in a number of countries has also shown that the severity of pain is not the only reason people get troubled by it. There are often times when someone can have quite severe pain, but manage to not get distressed about it. Equally, it is possible to get distressed about pain even when it is quite mild. Look at a section of a letter we received from one of our former patients (we’ll call her Jane).
Jane lived on a farm with her husband. Her persisting back pain had greatly limited what she could do around the farm. She was most concerned about not being able to ride her horses, either on the farm or in shows. During the time she participated in our programme she always stated that getting back on her horses was her main goal. We were more cautious and thought it would be too difficult (it would stir up her pain too much to be acceptable). After all, we believe that everyone with a chronic pain condition is likely to have some limits on what they can do. Accordingly, we encouraged her to think about less physically-demanding activities - ones which wouldn’t aggravate her pain as much. But she stayed determined to do it.
During the programme Jane made good progress, paced up her exercises and ceased all her pain killers. Her mood also improved. She returned home to put her new skills into practice. She had a difficult time because her husband wasn’t well and she had to help with many of the physically-demanding chores. But a year after leaving the programme she wrote to us to say:
“we have been doing a little every day rather than all in a couple of days. I have to say that I feel as though I am thriving on it. I have been horse riding again, which I thought I would never be able to do, though it was my number one aim, and today was absolutely brilliant! Chasing bulls up and down hills, into and out of creeks and dams at full speed, on such a magnificent Autumn day, is what makes life worthwhile! My pain level was very high, especially afterwards, but hey, the day was great!
Twelve months down the track, and it was a very hard track, I can move freely, easily, endure the pain much better and actually plan activities. Best of all, I can ride those beautiful horses and it feels as though there was no five year break!”
Jane still takes a little medication at times for her pain, but she described the amount “as minute in comparison” to what she used to take. At the same time, she described having “a huge increase in my physical abilities”.
What this shows is that despite doing something which did aggravate Jane’s pain, she didn’t become distressed. As she said, being able to ride again was worth more to her. She knew she wasn’t causing herself any damage and that the increased pain after riding wouldn’t last too long. She felt in control - after all, she knew that by riding her horse, especially in that vigorous way, she would make her pain worse, but she chose it. She also knew that if she paced the rest of her daily activities on the farm she could keep her pain under reasonable control - without relying on pain killers alone (as keeping her mind clear helped her to cope and to feel in control).
So that is a case of someone who is in a lot of pain but feeling happy. Earlier, before Jane attended the programme, she had been quite distressed when her pain was that severe. She was also much more disabled then and taking much more medication. When she first came to our clinic she was moderately depressed, but her pain ratings were no worse than they were when she was riding her horses.
So, by itself pain doesn’t have to make us unhappy, frustrated, irritable and all the other negative feelings that often go with pain. You can check this yourself by keeping a small diary of your pain levels over a few days, along with a record of how you are feeling (happy, sad, frustrated, angry or whatever), the sorts of thoughts you are having at these times and the situation you are in (what you are doing or where you are). Copy out the recording sheet printed here into a notebook and carry it with you for a few days. Whenever you feel your pain is getting worse, stop what you are doing for a moment and write down:
(1) your pain level (on a 0-10 scale, where 0 = no pain and 10 = worst pain imaginable),
(2) the thoughts you are having about your pain (like “not again”, “this is hopeless, I can’t go on”, “I must have overdone things, I’ll just take it easy for a while”, or whatever),
(3) how you are feeling (like happy, sad, angry, worried, or whatever). and
(4) your situation (what you are doing, or where you are, like driving the car, sitting at a desk, or whatever).
It is more helpful (and accurate) if you record your responses as close as possible to the time you feel your pain getting worse. If you leave it to the end of the day, your memory may not be as accurate.
We also recommend that you try not to read the rest of this chapter until you have made your own record of your responses to increased pain.
Try to make at least 10 entries in your diary, then have a look at what you have recorded.
Pain Response Diary
|
Date |
Pain (0-10) |
Thoughts (whatever is on your mind |
Feelings (happy, sad, etc.) |
Situation (where, when) |
|
Example |
7 |
What’s the use? Nothing works. can’t go on like this. |
despair, hopeless |
woken up, 2 am, I in bed |
Reviewing your diary
To begin with, look at the ways you have reacted (your feelings) and the pain levels at the time. Do you always react in the same way? Or does it change with different pain levels?
What else changes? Have a look at both your thoughts and the situations. Do you notice any links between your thoughts, your feelings, your pain and the situations you have been in? What might that suggest?
Now read the rest of this chapter. While you are reading it we would like you to think about your own pain and what you wrote in your pain response diary (as well as other times when your pain has been troubling or distressing you). It can help to discuss these issues with someone who knows you quite well as they may be able to act as a reasonably objective sounding board.
Helpful and unhelpful ways of thinking about pain
Remember the diagram in Chapter 1 (What is Chronic Pain?) of how chronic pain can lead to excessive suffering? If you can’t recall it, turn back to Chapter 1 and have a look. One of the boxes in the diagram mentions unhelpful thoughts. You might have wondered what this meant. After all, many people who have chronic pain tell us that they think in negative ways because of their pain. They say that if their pain was relieved these negative thoughts would disappear too.
Negative reactions to pain appear quite normal responses. Some patients who come to our clinic tell us that anyone in pain would feel like that or think like that, and that if only we had pain we would feel like that too. No doubt there is some truth in these statements. But are they always true? Does it have to be like that? Do we have no choice in how we react to pain?
The story told by Jane shows us that we can be in a lot of pain but also be very happy and full of life. Another patient who attended our clinic can show us a different angle. This patient (we’ll call him Joe) had previously had back surgery (a spinal fusion) and as that had not relieved his pain he later had a dorsal column stimulator implanted in his back. He told us that the electrical stimulation from this device had reduced the severity of his pain by 50%, but it was still about 5 out of 10. Despite this improvement, he continued to take strong pain killers (Opiates), he remained quite disabled at home, he was walking with the aid of a stick, and his mood was still very unhappy and often angry. He was especially angry about the unhelpful ways in which he felt he had been treated by his various doctors, his former employer and the workers compensation insurance company.
Joe was invited to attend our pain management programme. Initially, he was very skeptical. He couldn’t see how it could help him. He felt he was doing as much as he reasonably could and if we weren’t going to be able to take his pain away, then he couldn’t see how the programme could help him. Still, he agreed to come. Although he had some difficult moments during the programme, when he had some heated disagreements with the staff (who he felt were not listening to him and were pushing him too much), he completed the whole three weeks. By the end of the programme, Joe said his pain was about the same as it had been before the programme, but he was doing many more exercises, he was walking without a stick, his mood was much more positive, he was much more confident that he could do things despite pain and he had stopped all his medication. He could even share jokes with the staff.
We have kept in touch with Joe since he left the programme and that is now over 4 years ago. He reports that he still has his pain, but it is a lot less (mostly only about 2 out of 10), he still uses his stimulator (but only for about 15 minutes a month), he hasn’t taken pain killers on a regular basis for most of the last 4 years (and no opiates at all), his mood is generally very positive and stable (he is no longer easily angered), he keeps himself active around the house and he’s doing a technical course with the aim of finding work again. Joe has even started playing golf again and he has taken up fishing again. By most measures we would say that Joe has successfully learned to manage his pain, and he would agree. Along with other graduates of ADAPT, he even comes to the clinic from time to time to talk to new patients about his experiences.
How did he do it? Well, to begin with Joe felt that unless his pain was relieved by at least 50% he would not be able to get back to a more normal lifestyle. After he had the stimulator implanted he found that even with 50% pain relief things weren’t that much better. It was at that point that we talked to him about his role in managing his pain. Clearly, Joe couldn’t rely totally on the stimulator to do it for him. One of the critical things he started to realise during our pain programme was that his reactions to his pain and to others were actually contributing to how he was feeling (his anger, his depression) and it was not just his pain that was doing it. Joe was also using his medication to block out his negative feelings, but they were also making him feel worse.
When we looked at Joe’s pain response record in which he recorded his responses to increased pain we noted that when he was feeling distressed and angry, it was related more to his thoughts than to his pain. Thoughts like “this is hopeless”, “I’ll never get anywhere”, I can’t go on like this”, “what’s the point?” were usually linked to his distress and anger. His pain ratings went up and down, but his mood was worse when his thoughts were more negative and hopeless.
In other words, just as Jane had shown us earlier that aggravating your pain doesn’t have to make you feel depressed, Joe has shown us that getting good pain reductions doesn’t always mean we’ll feel a lot better and be able to do a lot more. Both cases show us that how much pain affects us and what we do is strongly influenced by the ways we think about our pain.
Importantly, our thoughts are under our control. We can choose how we think. We might get into habitual ways of thinking at times, and we may feel we have no choice, but we can always change our minds.
With this realisation, Joe was encouraged to test out our method of improving his mood and changing the whole way his pain was interfering in his life. Despite his initial doubts, he has shown it is possible.
How did Jane and Joe do it?
(1) First they came to see how the ways they thought about themselves, their pain and other people were playing a major role in how they felt and behaved.
Thoughts are not just a running commentary on what you do - they play an active role in influencing your feelings and behaviour.
For instance, it is easy to react to activities which may cause more pain by thinking in a gloomy way. Instead of looking forward to seeing friends, or doing something enjoyable, you may find yourself dreading the travel involved, or the sitting or standing, and it may all feel too much effort when you have the pain to cope with as well.
These thoughts will probably make you feel more distressed than if you hadn’t thought like that. Thinking like that may even make you change your mind, and give up the thing you had been looking forward to.
On the other hand, if you decided that the best way to deal with it was to “think positive” and ignore the pain you might just push ahead anyway, without planning, regardless of the consequences for yourself. But when your pain was aggravated, as is most likely, you could then say something like “see, I tried thinking positive and ignoring the pain and it didn’t work”. But is that the only way to look at what you did?
Or you might go, but be so worried about how you would feel by the end of it that you couldn’t enjoy yourself. In this case, you might say “well I did it but I don’t feel any better, so it was a waste of time”. Again, is this the only way to look at what you did?
If you are starting to think “this doesn’t apply to me”, put it to the test. For the next few hours, tell yourself every few minutes: “there is no point in trying to manage my pain. I feel dreadful”. How do you think you will end up feeling? If you don’t think it will make any difference, why not try it? On the other hand, if you think it will make you feel worse, it will help you to see the possible effects of such thinking on your feelings.
Ways of thinking can also become habits, just like ways of doing things. And like other habits, some ways of thinking can become unhelpful. And like all habits, unhelpful thinking habits take an effort to change.
You may find it hard at first to see how you can change the ways you think and feel. Many people believe that they have no control over their thoughts and feelings - that they are just made like that. But in the past you must have thought things over to make a decision, or changed your mind about something, or kept your temper when you felt angry. How did it happen? Through hearing what other people said, perhaps, or thinking of the possible consequences of reacting in another way?
(2) The second important step is becoming a good listener to yourself
Most probably, you can recall having changed your mind about something after listening to yourself, and talking things through with yourself. This can also happen when you talk things over with someone else. Remember when you have explained a problem out loud, to someone who listens carefully, only to find that you solved it as you talked, and felt much more hopeful (and pleased with yourself!).
Getting things clear is often the start of feeling better and managing better. You can become a good listener to yourself.
(3) Identifying helpful versus unhelpful thoughts
Having a few worries and even a degree of unhappiness is a normal experience for all of us from time to time. But repeatedly becoming very worried or anxious or depressed for extended periods is not normal. In most instances we should be able to identify thoughts that are contributing to these more distressing emotions.
Often people describe their thinking at these times in terms of “positive” or “negative” thinking. These are terms most of us understand, but it often difficult to pin down exactly what they mean. As a result they can be misleading. For example, “thinking positively” can be OK at one level, when there are no major threats or problems. But when there is a major threat (like the development of a dark spot in your skin which could be a sign of skin cancer) simply thinking positively could result in your ignoring it and hoping it will go away. In this case, positive thinking will not be helpful in sorting out the problem. So thinking too positively can amount to denying that there is a problem. As a result you may not develop an effective plan to deal with a real problem. In the case of chronic pain, such thinking could result in your overdoing things and making your pain worse than it needs to be. Positive thinking may help to keep your spirits up, but it is not usually enough for good problem solving.
Negative thinking is similar to positive thinking in that it could be quite inaccurate, but in the opposite direction. So thinking negatively could mean that you think nothing will ever be any better. Such thoughts are likely to be obstacles to your even trying to have a go at doing something.
Of course, there are often a number of ways to look at most situations. There’s a common saying that there are always two sides to every story. In fact, there could be more than two sides. So, there are often many ways in which you can deal with a problem, but some will be more effective than others.
Rather than talk in terms of “positive” or “negative” thinking when trying to deal with real problems like living with pain, it can be more useful to talk about “helpful” versus “unhelpful” thinking.
Helpful ways of thinking are those which enable you to deal effectively with a problem or source of stress. Helpful thinking may not solve all problems, but it should allow you to make some progress. In contrast, unhelpful ways of thinking are those which cause you even more distress. Unhelpful thinking may be understandable, but not helpful. For instance, when you are in a lot of pain it would be understandable and even accurate if you were to think your situation was terrible and completely unfair. But would it help if it led you to feel even more distressed? On the other hand, it might be more helpful if you were to acknowledge that your pain was severe, but at the same time to say to yourself that the best way for you to deal with it is to stay as calm as possible and avoid extreme reactions, reminding yourself that you’ve had pain like this before and you know it will pass and you will be OK. Such thinking could help you to minimise your level of distress and to feel more in control.
Helpful thinking doesn’t mean telling yourself you are not in pain or that you don’t have any problems. That might be called “positive thinking”, but it is only denying real problems and while it might buy temporary comfort, you can’t kid yourself forever.
As a rule, helpful thinking will be reasonably accurate. You will usually deal with a problem more effectively if you can assess it accurately. Accurate assessment can allow you to prepare for a challenge or stress appropriately. Overly positive assessments of problems risk underestimating the size of the task facing you. Equally, overly negative assessments risk overestimating the size of the task.
So, if you find yourself becoming increasingly agitated over your pain spend a few moments checking on your thoughts. Are they helping you to cope or are they making you feel more distressed? If they aren’t helping, even if you feel they are justified, they must be challenged.
Here are two examples of how common reactions to pain can build into major self-defeating events if left unchecked.
(1) When worry grows into anxiety and then panic
We all worry at times - in fact, a little worry helps to keep us safe from taking unwise risks. But when it goes on and on, and leads to unwise decisions, it’s no help at all. The following diagram shows the sort of vicious circle that can develop.
For example: Think of being in a difficult situation, such as at a crowded supermarket or in a car on a busy road, and you feel your pain is getting worse….
What if your reactions were like these?
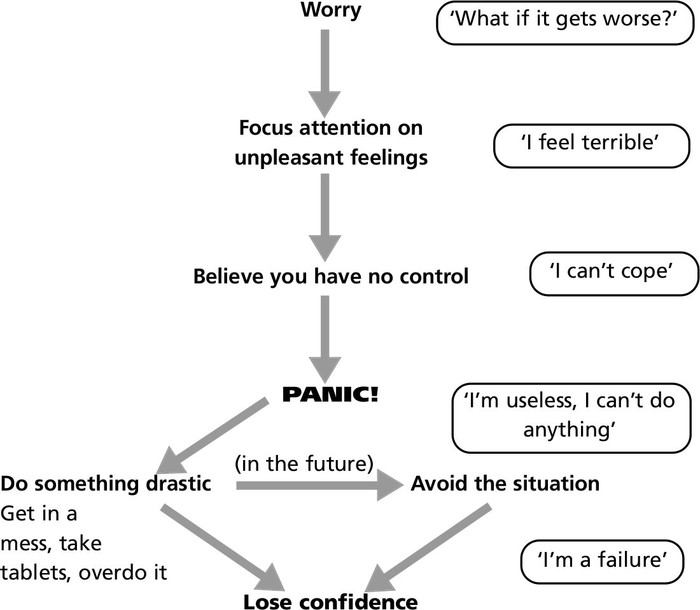
Try following the arrows through, remembering the last time you got into difficulties when your pain flared up. These are common reactions, but there are other ways of reacting the are more helpful.
In general, people get panicky when:
· they believe the threat or possible harm is greater/worse than it is,
· they think they are very likely to come to harm,
· and they forget how they can cope.
So, at times of difficulty with your pain, you need to check -
(1) Are you being realistic about the risk? For instance, if your pain is increasing, how likely is it that it will become unbearable and lead to something awful? (how often has it really got like that before?)
(2) even if the worst happened could you cope? For example, do you find yourself worrying that it could be terrible and that you won’t be able to cope with it? Or do you start worrying that it might be some undiagnosed and serious disease, and start to picture yourself bed-bound, helpless, or worse?
Or do you think to yourself about all the other possible (and less serious) reasons for it worsening, and about what you can do?
Focussing on feelings
When you are feeling anxious, frightened, or panicky, you are probably focussing on the things you fear - such as collapsing, or breaking down in public, or losing control. On the other hand, when you are feeling calm, you probably won’t be thinking like this. In fact, when you are feeling calm, you may think you were being “silly” when you were feeling anxious or panicky. When you stay focused on what you’re trying to achieve or do and not how you feel, you are more likely to feel calmer.
To help you see how your thinking can affect your feelings, try the following exercise:
Think of an anxiety-provoking situation that you have experienced with your pain. Replay that situation in your head - from start to finish - to recall the fears you felt at the time. Then - staying calm - try to work out how likely those fears were. (For example, would you really have collapsed? And even if you did, would no one have helped?). It is also quite likely you would have coped successfully before with this sort of situation. Look at the effect of reminding yourself of that.
Your confidence is also important when it comes to dealing with fears and worries. Unfortunately, you can’t just get confidence without any effort. What other people say can make you feel more or less confident about how you cope. But what you say to yourself will make the biggest difference. When things go badly, do you criticise yourself? Do you tell yourself you are “useless”, “hopeless” or “stupid”? If so, stop and ask yourself….
Am I being fair to myself?
Is it helpful to think like this?
The answer to both is - NO. This sort of thinking is undermining you. Imagine how you would feel if someone else said it to you.
To think about it another way. When you do something well, how often do you tell yourself you are “clever”, “brilliant” or “capable”. Most people say they don’t do this, but they are quite prepared to say very negative and critical things to themselves when they make a mistake. If you treated someone else in this way, say your children or friends or even your dog, what might be the result? So why do it to yourself?
Remember the example of the leading sports players that we see on TV. When they do something well, whether it is a fast time, a good kick or they save a goal, they usually show how pleased they are - they recognise their achievements. Equally when they make a mistake they try to work out where they went wrong and how to do it better next time. The successful players don’t waste time getting into a stew over their mistakes - they try to learn from them and avoid repeating them.
The same methods can be used in coping with pain.
Confidence comes from doing things as well as possible - recognising it yourself - and remembering it - and telling yourself (and even other people) about it.
Coping with your pain, and carrying on as normal a life as possible despite it, are things you know how to do well. When you feel your pain getting stirred up, stopping to think and plan your next step instead of panicking is a success in itself. If you expect yourself to manage perfectly, you will rarely be satisfied. If you are realistic about what you can manage, and achieve it, or get some way towards it, you have every right to be pleased. And when you are pleased with your achievements, you will gain confidence.
So how about undoing the vicious circle to make it look like this:
When you start to:
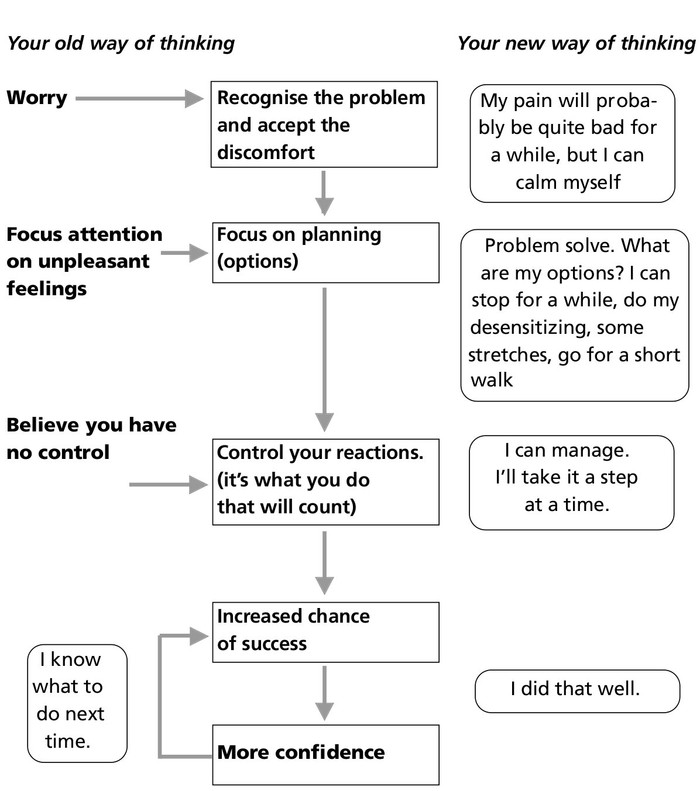
More Helpful Reactions to Increased Pain
Try these methods out on yourself. You may find it useful to start by remembering a recent occasion when you had difficulty coping with your pain. Think about how you managed it then and how you might manage it now using the methods outlined here. When you feel your pain is starting to bother you again try these methods out and then review how you managed. What can you learn from your first attempts? How could you do it better?
If you are finding it difficult to master by yourself, it may be helpful to work on these methods over a few sessions with a clinical psychologist. They are specially trained to help people in this way.
(2) Accepting that your pain could last a long time
No one wants to live with pain. Coming to terms with having chronic pain and accepting you may have to live with it for a long time is hard for everyone who has it. If your doctor says there’s no cure for your pain and “you will just have to learn to live with it” he or she may not tell you how to do that. You might think “well it’s all very well for him or her, they don’t have pain”. You are also likely to refuse to believe your doctor is right - maybe if you keep looking you will eventually find a doctor who can fix you. You may think something like “after all, ‘they’ can transplant hearts and kidneys and do all sorts of wonderful things, so surely ‘they’ can fix my pain?”
Possibly because of all the news and information we get these days it often seems that we have come to almost expect all health problems to be solved or be close to it. Almost daily we hear of “breakthroughs” in the fight against some disease or other. However, if you keep listening you will also often hear that the study was done on rats in a laboratory and it may be 5 years or more before the new treatment will be available to humans.
For some time you are likely to view your pain as “acute”. You will say to yourself things like “it’s only been a short time since I got it and it’s bound to settle soon”. But those weeks can become months then years. It is true that pain conditions like back pain usually wax and wane over time, but for many people it never goes away for long. For others, some pain will be present most of the time but every now and then it will get worse for a period. Over time, the periods when it is worse may become more frequent. If you keep waiting for the pain to go away, or for someone to take it away for you, it is likely that you will have a long wait. In the meantime, what is happening to your life? Your family? Your work? Your friends?
Recognising these effects is an important part of coming to terms with your pain. It can help you to start problem-solving and stop waiting for something to happen.
It is likely that you will have tried try to keep up most or all of your normal activities - at home, at work, in your sport or social life. But if these activities make your pain worse you are likely to start finding many of these activities become disrupted by the pain. Some will push on regardless and suffer more pain as a result, as we discussed in the chapter on pacing. Others will stop what they are doing and may start to avoid many activities which aggravate their pain. At these times you may say to yourself things like, “I’ll take it easy for a while and things might improve”. You may even get advice from your doctor or physiotherapist to “let pain be your guide” - or whenever you do something which makes your pain worse, stop that activity. That can be acceptable for a few minor tasks, especially if there’s someone else to do it for you and you never really liked doing it anyway, like washing the dishes or doing the grocery shopping.
However, as we discussed in the chapter on the effects of pain on your lifestyle, cutting back on normal daily activities can lead to deconditioning of your body and to your putting on more weight. This, in turn, can lead to more pain. It can also lead to frustration, especially if you start to think about all the things you have given up or can’t do as well as you used to. In fact, not being able to do something you would really like to do, especially if it is due to pain and that pain was due to something that was not your fault, can lead to a great deal of frustration. Over time, it can lead to resentment. You may wonder what you’ve done to deserve this. Some people us that they feel it is almost as if they are being punished for something.
When you keep trying to put the pain to oneside and to get on with your life, but you keep having set-backs and feel you are not getting anywhere, you might also start to feel hopeless or despondent. You may feel that you will never get on top of it.
Equally, when you repeatedly get your hopes up about a new treatment or seeing a new doctor or clinic, only to have them dashed, it is likely you will start to feel helpless or even desperate. Many patients at our clinic tell us that they are prepared to “try anything”. To us it often seems that people with chronic pain who keep seeking treatments which keep failing are like people who have been unemployed a long time and have had repeated knock-backsfrom prospective employers. And, of course many people with chronic pain are unemployed and that will often make their problems even worse. After having these sorts of experiences for a while, it is not surprising that many people with chronic pain start to feel helpless and depressed. Eventually they may feel despair at the prospects of anything ever improving again. Some may feel that life is not worth living anymore.
The despair that can come with repeated treatment failures is often coupled with a sense of loss. The sense of loss is usually to do with having had to give up activities that were enjoyable and gave life some of its meaning, such as work, sport or just going fishing. The sense of loss can also be related to loss of feeling well and healthy or robust. In some ways, aspects of loss for people with persisting pain can be like the loss that we all feel as we age and can no longer do the things we used to do or no longer look so young and fresh. Yet we often hear people saying that they would like to grow old gracefully. That means accepting that you are getting older and seeking out the opportunities that aging can provide. In contrast, others refuse to acknowledge they are aging and seek to appear as young as possible, often doing the things they couldn’t afford to do when they were young.
If you find yourself getting into these situations, what are your options?
Well, it can help to talk such feelings through, with yourself or with someone else, to get a more balanced view. One of the difficulties is that the memory plays tricks when you are depressed. This can make it easier to remember unhappy events and the times when you have not coped, and harder to remember much about times when you have managed well. This means you have to make an extra effort to think it through clearly.
It is important to realise that some sadness at times (but not all the time) is a normal reaction to having persisting pain. After all, no one usually wants to live with pain. So try not to be too hard on yourself if you do feel a little low at times. However, if you find yourself starting to feel low for much of the time and you’re having trouble pulling yourself out of it, then it probably is time to do something about it.
It can help to write down your thoughts, and your feelings, especially when you are feeling a bit gloomy or your pain is getting worse. Try to see where these thoughts and feelings lead.
For instance, you may be looking around at the house or garden … you notice something that needs doing … then you think about the difficulties of doing it … and about the increased pain it could cause … and you start to tell yourself that things around the house are getting in a state … you couldn’t ask anyone round because of it but you can’t go out to see friends because of the pain … so you won’t see anyone … you’ll be trapped indoors getting frustrated at it all … it hardly seems worth getting up in the morning … what is there to look forward to, and so on.
What started with noticing a job which needed doing has quickly led downhill to feeling that life is hardly worth living - and this can happen in a few seconds. In fact, you may well not be aware of the thoughts, just of the feeling of complete hopelessness, and it will seem as if it came out of the blue. But it didn’t come out of the blue. Your thoughts led you to that point, and the best way to begin to catch these streams of thoughts is to write them down, and to think about them. That is the first step to being able to stop them, and to stop yourself from feeling like that. After all, if you read back through the thoughts, they are not the whole picture. What you should be aiming for is realistic, helpful thinking.
It is harder to do this when you are feeling extremely distressed. It is much easier to catch yourself slipping - starting to think in unhelpful and increasingly desperate ways - early. If you wait until you feel extremely hopeless before you try to drag yourself out of it, it will usually be much harder than if you’d stopped yourself getting to that point.
If you find yourself repeatedly getting frustrated or depressed about your pain there are some relatively simple steps you can take to get things back into balance.
(a) First you need to identify the sorts of thoughts you have at these times.
(b) Then you need to examine them carefully, and see if they are a fair picture.
Remember that it can be hard to remember the more positive things in life (including your own strengths and qualities).
Start early: it’s much harder to tackle the despair at the end of the line than the partial picture at the beginning.
Taking the example given above, you could ask yourself questions like:
… does this job I have noticed really need doing? … is it urgent? … am I the best person to do it? … What about help from others? … if I am going to do it (with or without help), does it have to lead to increased pain? … What about pacing, or preparing by doing some stretch exercises, planning how you could do it, and so on? … Is it really a higher priority than me? … if it’s not done, is it really true that the house is not fit to have friends in? … What sort of friends judge you by the state of your house? … Do you judge others like that? … and so on.
At each point, you need to ask yourself how realistic the thoughts are, and whether they are helpful. It can also be useful to remind yourself of how you have coped in the past, and how you learned to cope with your pain at times. Think about how you would help someone else who was thinking and feeling like this - would you be telling them that life was not worth living? (so why tell yourself things like that?)
What all this adds up to is REALISTIC AND HELPFUL THINKING.
Unrealistic and unhelpful thinking can be all negative, like the examples above. Or it can be expecting too much of yourself, setting such high standards that you will never reach them.
It can be helpful to ask yourself things like:
“What is the worst that can happen?”
“Would it be so awful that I couldn’t cope at all?”
“How likely is it anyway?”
“How might you deal with it if it did happen?”
Once you have answered these sorts of questions, you will be in a good position to handle even the worst situation.
Unrealistic thinking can also be too positive, denying that there is any problem, and setting you up for overdoing and failure.
After all, if someone else tells you to “cheer up and forget about the pain”, you probably, quite rightly, feel angry and misunderstood.
Ignoring your pain as much as possible and trying to act as if it wasn’t there can work for a while. But in the end you won’t be able to kid yourself about it forever.
For example, one lady who came to our clinic told us that during the week she tried to keep herself as busy as possible at work and at home. This helped her to not notice her pain for much of the time. But often on the weekends when she was trying to relax she found her pain was worse than ever. When she tried to pace her activities more effectively during the week, she found she had less pain on the weekend. This meant that by acknowledging her pain she was able to develop ways to get around it. Whereas before she had denied the existence of the pain and paid the price of that each weekend.
While it doesn’t help to think about your pain all the time, it also doesn’t help - or not for long - to simply tell yourself just to get on with it and forget the pain. Pain patients often talk about “fighting the pain”. But who can win, when the pain is yours? Who loses? How long can you keep this battle up?
Perhaps it would be more effective to use your strength to negotiate with the pain over what you can do, and how you will do it.
Helpful, realistic thinking is accurate, balanced, and gets things in perspective - not just looking at the problems, but also about the resources you bring to the problem: a good brain, ways of managing pain, and a reasonably fit body.
Helpful thinking means that you are as clear as you can be about your limits, but they don’t overshadow all that you can do within them. It means that you appreciate your past successes, and that gives you confidence for the future. It means that you can ask friends or family members for help which they can give, and offer appreciation and perhaps another sort of help in exchange.
Remember, these ways of thinking are all habits. They are not easy to change - but they can be changed. And they won’t change on their own, nor will tablets take them away. In fact, people who take tablets to calm them down, or brighten them up, tend to believe it’s the tablets working when they feel better, but blame themselves when they feel worse - so there’s no way to win with this approach!
You may think that this is all a bit unnecessary - like icing on the cake. But years of helping chronic pain patients to change their lives has shown that working on the way you deal with your thoughts and feelings is as important as working on exercises. Making changes, getting fit, feeling better and achieving more doesn’t last unless you recognise that it is due to your efforts - not just the doctor or physiotherapist you have been seeing. After all, if you put all your improvements down to others, it would make it hard for you to keep going when they weren’t around.
Some points to remember:
· When you are not managing so well, try to remind yourself that you have the means to get back on course - by challenging the worries or the hopelessness, and changing them.
· If you put your successes down to chance, it will be harder to make steady gains, and to look forward to what you can make of your life.
· If you are too hard on yourself when you make mistakes or if you set such high standards that you are bound to fail, progress will be that much harder
Challenging unhelpful thoughts
When you are aware of feeling irritable, anxious, hopeless, or miserable … stop and listen to what you’ve been saying to yourself. Try writing it down (use the recording form shown earlier in this chapter). Read through the examples in this chapter, and use the questions suggested. You may find yourself feeling a certain way at particular times - maybe when you can’t sleep, or before exercise, or when you are bored with what you’re doing.
When you are ready, have a look at what you’ve written. Ask yourself about the thought:
“Is that a fair judgement or statement?” and
“Is it helpful to think like that?”
You could also ask yourself:
“Are there other ways, more helpful ways, I could look at this?”
Underneath your initial, unhelpful thoughts write down the answers to these questions, or anything else that helps you to get things in perspective. Also write down any feelings associated with these new thoughts.
For example,
One patient who attended our programme wrote that when he had thoughts like “this is hopeless” “I can’t go on” “The pain’s unbearable”, he felt depressed, hopeless.
Then he challenged these thoughts by saying things like:
“well I’ve had pain like this before and I have managed” “I know I’ll be OK, I haven’t injured myself again, so it will settle”. “I’ll work out a plan to get through the next little while” “I’ll take a step at a time, cut back on the more vigorous activities, but keep doing things I can manage”; “the pain is quite bad, but it’s been like this before and I know it will settle sooner or later”. When he had thoughts like these he reported starting to feel back in control again.
Of course, he had to keep doing it. But that’s no different to cleaning your teeth. We all know that if we stop cleaning our teeth we are likely to have trouble with them. So we take care of our teeth and prevent problems by taking a few minutes each day to clean them. The same approach can apply to managing chronic pain.
If you keep checking for unhelpful thoughts and reactions to pain, and challenging those thoughts when you spot them, your mood will be under your control much more (rather than being controlled by your pain).
With practice, it get easier. Remember how learning to drive, or cook, or sew or do carpentry seemed almost impossible at first - and still look pretty complicated to those who can’t do them. They took lots of concentration and practice. You would also have tried to learn from the inevitable mistakes you made. But after a while, you could drive or cook while you talked, or listened to the radio, even though you were making complex decisions very rapidly in order to do so. Challenging and changing your unhelpful thoughts is just the same. It can become a very useful habit. The key is to recognise the unhelpful thoughts as soon as they appear - don’t wait until you are really down in the dumps before you start to challenge them.
We should emphasise that challenging unhelpful thoughts doesn’t mean trying to stamp them out or just blocking them - if you try these techniques you’ll find they keep coming back. Instead, challenging unhelpful thoughts means identifying other, more helpful ways to look at things and moving on with those. The unhelpful thoughts can be left to the side and you don’t need to waste energy on them.
Further reading
If you would like to read more about this way of dealing with emotional problems we would recommend that you find “Beating the Blues”, by Susan Tanner and Jill Ball, two clinical psychologists from Sydney.
If reading this book or others like it is not enough, then we would recommend that you ask you local doctor to recommend a psychiatrist or clinical psychologist with expertise in this area. If persisting pain is the main problem then we would recommend that your doctor refer you to a nearby multidisciplinary pain clinic or centre for a full assessment.